Recently, a top journal in the field of Electronic Health Record (EHR) development posted this quote from an anonymous doctor who was dissatisfied with his EHR:
“I firmly believe this EHR makes important information difficult to find and interpret, and it is very inefficient.” He went on to say, “It creates superfluous and difficult-to-navigate notes and information that are not centralized. That makes it easy for care providers to disregard notes, and they often do. That affects patient safety. . . . It is difficult and arduous to document in the EHR, and providers’ efforts to do so still yield subpar results with erroneous, irrelevant information.” 1
This doctor is pointing out a very real problem inherent in some EHRs. However, he was referring to one of the “ONC Certified” EHRs which we’ve discussed previously. Those types of EHRS are inherently much more difficult to use than most EHRs that have been specifically created for the mental health professions, such as PSYBooks.
The screenshot below is PSYBooks’ digital chart for a fictitious patient named Jake Conner. It has tabs across the top to keep everything organized, just like the nicer paper charts do. Notice that the last tab on the right is called “Notes” and it is exactly the kind of centralized repository for patient notes that the doctor above was wishing he had:
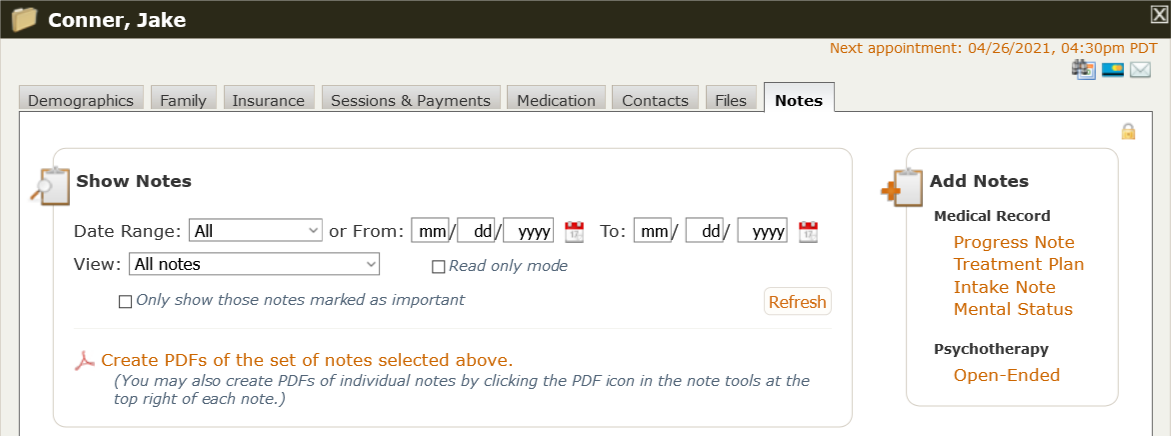
By default, all notes pertaining to this patient that have been collected on any form in PSYBooks are displayed on this page. However, practitioners can refine the notes they view with the various filters shown above, including using the “View” dropdown to see one of these broad categories of notes: All notes, Only medical record notes, Only psychotherapy notes or Specific medical record notes:
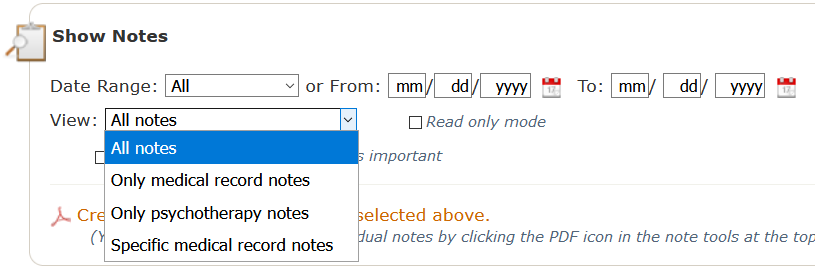
If you choose the Specific medical records notes category, you’ll be able to further refine your view with a screen like this:
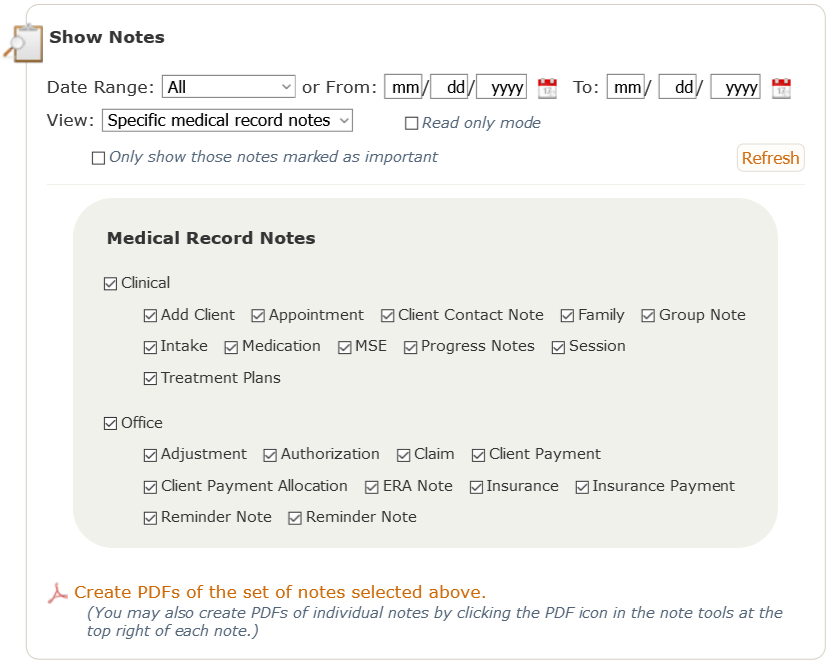
Once you’ve chosen which notes you want to view (the default is “All”), the notes you selected are displayed below this top filter portion of the notes page. A full page of notes on a patient’s chart might look something like this:
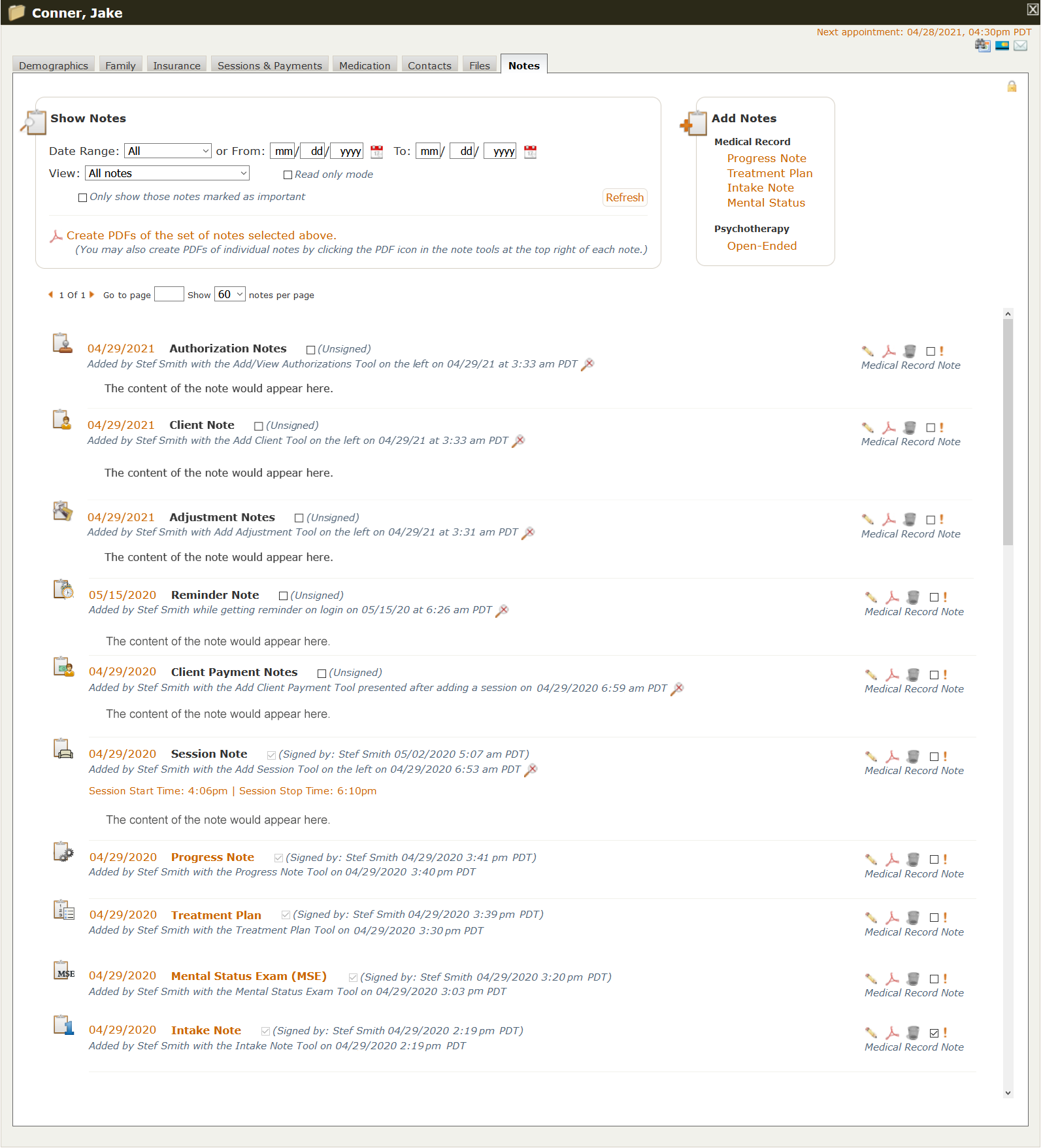
There are several things to notice on this page. First, each note type has its own icon, to help you more easily identify them. Here are some examples of note icons used in PSYBooks:
![]()
Also, more involved, structured note types such as Intake Notes, Mental Status Exams, Treatment Plans and Progress Notes are presented as links (indicated by orange text in PSYBooks). For example, the screenshot below shows an example of what you might see if you clicked a Progress Note link:
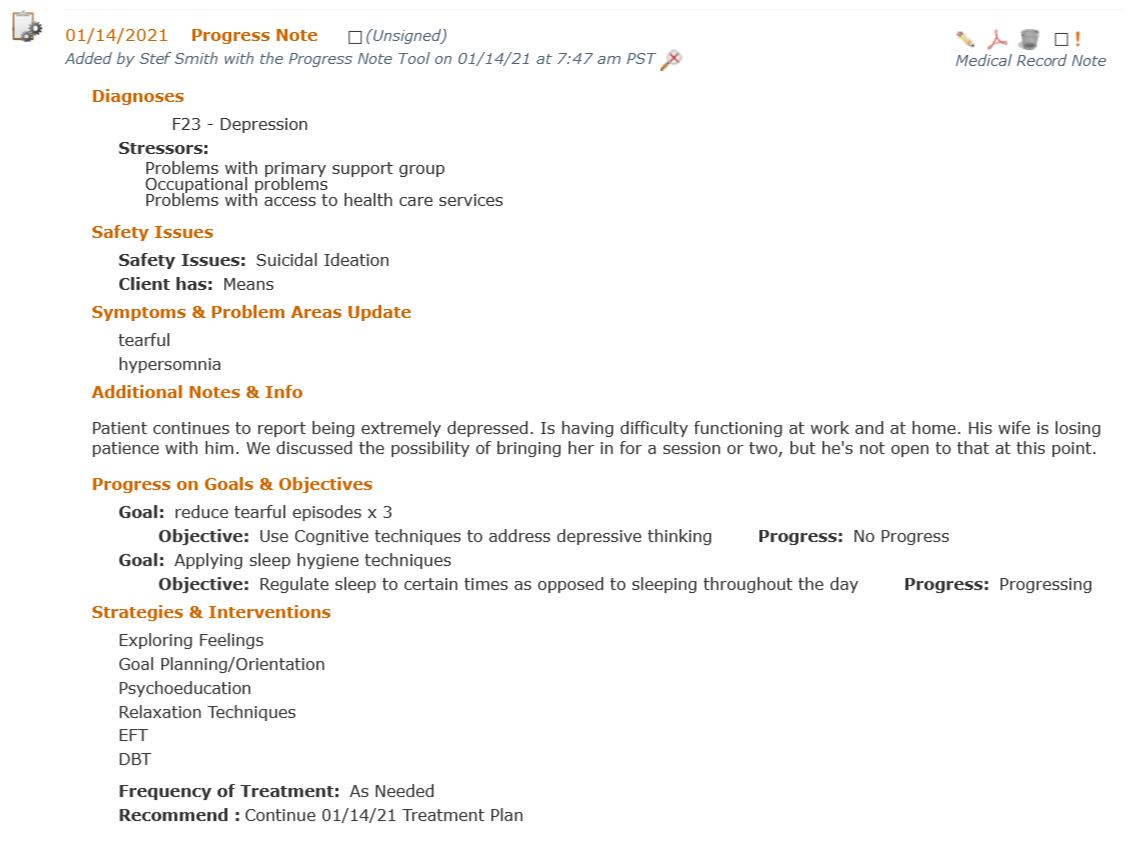
Also, notice that PSYBooks automatically signs and dates both when the note is entered and also when it is signed, which can be helpful in situations where you may need this kind of documentation. Session start and stop times are also added automatically. Finally, on the right hand side of each note entry, you have this set of tools:

These tools allow you to do the following:
- Edit the note if you haven’t yet signed it or add a revision if you have.
- Convert it to a PDF. This allows you to send it via encrypted email to the client, colleagues, or anyone else who may need it, print it, etc.
- Delete the note from this page. (Notice that all deleted items are tracked in the Activity Log, which means that there would still be a way to see deleted notes and other items should you need them.)
- Mark a note as important. This can be helpful if you have a patient who is in crisis and you want to be able to easily filter all notes related to the crisis.
- Under the tools is a label to let you see at a glance whether the note is part of the patient’s medical record or whether it’s an individual psychotherapy process note you’ve entered.
Part of why the anonymous doctor quoted at the beginning of this post could not see all notes pertaining to his patient is because in larger settings – or even small offices with admin staff – more than one person can add notes to a patient’s chart. Some EHRs will then only allow the person who wrote the note – or that “tier” of employee – to view it. However, PSYBooks handles this by putting all notes on one page but making it clear who wrote the note. In the example below, “Pam Jones” is an admin who has been taking care of getting authorizations for the therapist’s patients. In this case, she’s entered a note about a certain authorization that appears in the patient’s chart – which all will be able to view:
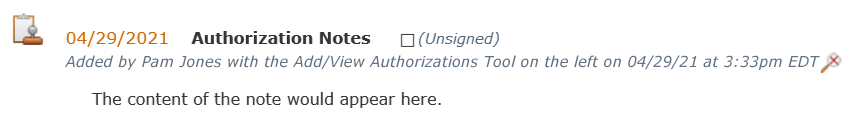
Want all your patient’s notes to appear in one place so you don’t have to search for them? We’d love to show you how it works! Schedule a demo or sign up for a free trial now!
1EHR Vendor, Organizational Relationship Key to EHR Satisfaction. (2021). https://ehrintelligence.com/news/ehr-vendor-organizational-relationship-key-to-ehr-satisfaction